Translate this page into:
Anterior neck swelling in a child: Cytological consideration of an uncommon diagnosis
*Corresponding author
-
Received: ,
Accepted: ,
This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms.
This article was originally published by Wolters Kluwer - Medknow and was migrated to Scientific Scholar after the change of Publisher.
A 4-year-old female child presented with a gradually increasing swelling in the lateral aspect of the right side of the neck for 9 months. There was no history of pain, fever, weight loss, or tuberculosis in the past. On local examination, swelling was about 4 cm × 2 cm in size, firm, and nontender with restricted mobility [Figure 1a]. Figure 1b–d shows the cytomorphological features of the fine-needle aspiration (FNA) in Giemsa- and Pap-stained smears.
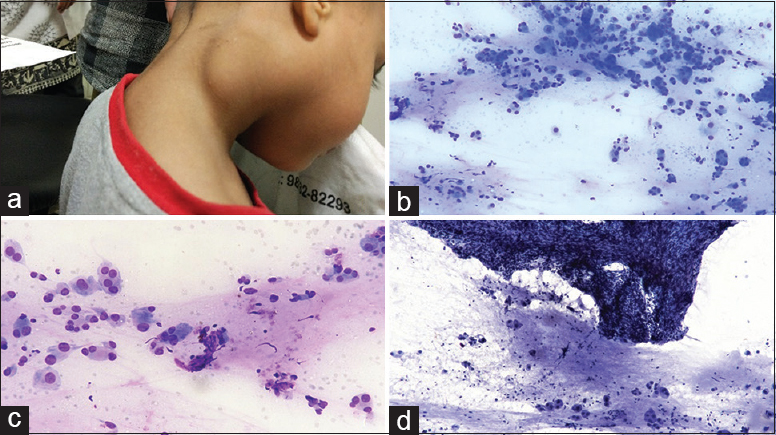
- (a) Right-sided subcutaneous neck swelling, (b) scattered large cells with few binucleate forms in a background of proteinaceous material (Papanicolaou, ×200), (c) large polygonal cells with central to eccentric nucleus, prominent nucleoli, and abundant cytoplasm (Giemsa, ×400), (d) fragment of spindle cells with slender nuclei embedded in a matrix along with scattered large cells (Papanicolaou, ×200)
QUESTION
What is your Interpretation?
-
Granular cell tumor
-
Paraganglioma
-
Ganglioneuroma
-
Acinic cell carcinoma.
ANSWER
The correct cytopathological interpretation is c:
(c). Ganglioneuroma (GN) is the most differentiated and benign form of peripheral neuroblastic tumors. Majority of pediatric cases occur in infants and young children <10 years and present as a solitary, slow-growing mass lesion.[1] The most commonly affected sites are the posterior mediastinum, the retroperitoneum, and the adrenal gland, whereas cervical region involvement is infrequent, with only 1%–5% of cases.[2] In the current literature, reports of GN's cytological appearance are scarce.[1]
In the present case, ultrasonography neck showed a solid well-circumscribed lesion measuring 4 cm × 3 cm × 2.5 cm in the superficial plane and not attached to underlying structures. FNA cytology (FNAC) was done from the swelling and revealed cellular aspirate. Smears prepared were air dried and fixed in 95% ethyl alcohol and subsequently stained with Giemsa and Papanicolaou stain. Smears were moderately cellular comprising large polygonal ganglion cells in groups, loose clusters, and many singly scattered. Cells had abundant granular cytoplasm, eccentrically located vesicular nucleus with prominent large nucleolus. Few foci of scattered mature lymphocytes were also noted. The background was hemorrhagic with areas of proteinaceous material.
Considering the age and cytomorphological features, possibilities considered were GN, granular cell tumor, paraganglioma, and acinic cell carcinoma [Table 1]. Periodic acid–Schiff stain was done and was focally positive, thereby not assisting in further diagnosis. On careful rescreening of the smears, occasional fragments of spindle-shaped cells with wavy nuclei embedded in a fibrillary matrix were seen and the neuronal cells with Schwannian stroma were also seen. Thus, a cytological diagnosis of GN was made.
| Features | Ganglioneuroma | Granular cell tumor | Paraganglioma | Acinic cell carcinoma |
|---|---|---|---|---|
| Age | Usually adults, children <10 years | 10-50 years | 30-50 years | 40-50 years Children uncommon |
| Common location | Posterior mediastinum, retroperitoneum, adrenal gland | Tongue, throat, chest wall, bronchus | Carotid artery bifurcation, middle ear, base of skull | Salivary glands; mainly parotid gland |
| Morphology | Large polygonal ganglion cells with prominent nucleoli. Background of Schwannian (fibrillary) stroma | Nests of large polygonal cells with granular cytoplasm. Nucleoli inconspicuous to prominent. Background hemorrhagic with scattered granular material | Nests of round to oval to polygonal cells, finely granular cytoplasm. Nucleoli +/- background hemorrhagic | Clusters, sheets and groups of bland acinar cells with eosinophilic granular to vacuolated cytoplasm. Prominent to inconspicuous nucleoli. Background hemorrhagic |
| Special stain/IHC | S 100+, synaptophysin+ | PAS +; diastase resistant S 100+ | S 100 +, Synaptophysin + | PAS +; diastase resistant |
IHC: Immunohistochemistry, PAS: Periodic acid–Schiff
On follow-up, excision biopsy was done. It revealed scattered mature and immature ganglion cells in the background of Schwannian stroma [Figure 2a and b]. Scattered lymphocytes were also noted. There was absence of necrosis, mitosis, or neuroblasts. On immunohistochemistry, S100 and synaptophysin were diffusely positive [Figure 2c and d] and a diagnosis of benign GN was made.
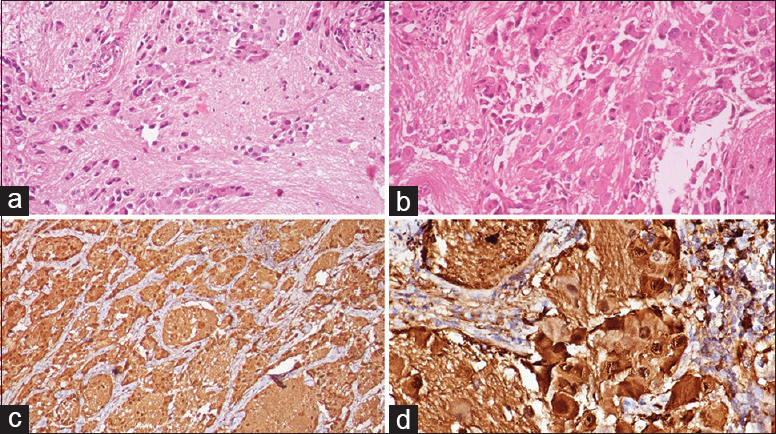
- (a) Scattered ganglion cells in a Schwannian background (H and E, ×100), (b) mature and immature ganglion cells along with scattered lymphocytes (H and E, ×400), (c) synaptophysin positivity (×200), (d) S100 positive ganglion cells (×400)
ADDITIONAL QUIZ QUESTIONS
Q1. GNs with syndromic association are seen most commonly at which site?
-
Retroperitoneum
-
Soft tissue
-
Posterior mediastinum
-
Gastrointestinal.
Q2. Cytological finding of ganglion-like cells is seen in which of the following?
-
Atypical lipomatous tumor
-
Nodular fasciitis
-
Schwannoma
-
Giant cell tumor of soft tissue.
Q3. The presence of ganglion cells and Schwannian matrix in FNA smears raises the possible diagnosis of which of the following?
-
Ganglioneuroma
-
Ganglioneuroblastoma
-
Neuroblastoma
-
Both a and b.
ANSWERS TO THE ADDITIONAL QUIZ QUESTIONS
A1. d; A2. b; A3. d.
A1. (d) GNs of the gastrointestinal tract may be associated with MEN 2B, neurofibromatosis 1, Cowden syndrome, tuberous sclerosis, and familial adenomatous polyposis. Cowden syndrome is a part of PTEN hamartoma tumor syndrome and multiple gastrointestinal hamartomas or GNs are among the major criteria for Cowden syndrome.
A2. (b) Atypical lipomatous tumor is a neoplasm characterized by the presence of lipoblast. Nodular fasciitis is a benign, reactive proliferation of myofibroblasts that can mimic sarcoma both clinically and morphologically. Nodular fasciitis may show pleomorphism with the presence of ganglion-like cells. Schwannoma has hypocellular component and cellular areas of spindle cells with verocay body formation. Giant cell tumor of soft tissue mimics its bony counterpart and shows numerous large multinucleated osteoclast-like giant cells along with mononuclear cells.
A3. (d) Among the tumors of autonomic nervous system, ganglioneuroblastoma affects mainly the pediatric age group and is an important differential of GN. FNAC cannot rule out the presence of focal neuroblastic component. Excision biopsy can only confirm the diagnosis. In neuroblastoma, immature neuroblastic component predominates. Rosette formation may also be seen.
BRIEF REVIEW OF THE TOPIC
GNs are the well-differentiated tumors of the autonomic nervous system. They are slow growing and frequently asymptomatic or may proceed with compression-related symptoms.[3] It is an uncommon soft-tissue tumor in the pediatric population and most commonly occurs in infants and young children <10 years of age, slightly more often in girls than boys with a female:male ratio of about 3:1.[4] GNs are typically located in the thoracic cavity in posterior mediastinum (60%–80%), the abdominal cavity (10%–15%) with involvement of adrenal gland, retroperitoneum, pelvic, sacral, and coccygeal sympathetic ganglia, and uncommonly in the cervical region (1%–5%).[56] Other rare sites reported are the middle ear, skin, parapharyngeal region, orbit, and the gastrointestinal tract.[789] GNs are easily recognized on excision biopsy. However, scarce data on cytomorphological diagnosis may pose a diagnostic challenge on FNAC. FNA smear of nerve sheath tumors are usually low to moderately cellular, containing cohesive elongated or spindle-shaped cells with slender wavy nuclei having pointed ends in a background of myxoid material. The most striking feature of GN is the presence of abundant mature ganglion cells having a large nucleus with dispersed chromatin and a prominent large nucleolus which was seen in our case. However, FNAC or core biopsy may miss the scant immature neuroblastic component; thereby, a complete resection is recommended due to prognostic and therapeutic implications.[1] It is important to differentiate them from pseudosarcomatous proliferations such as proliferative fasciitis and proliferative myositis as they may show ganglion cell-like cells on cytology.[10] However, the absence of Schwannian stroma and the clinical course of proliferative reactive lesions can aid in the cytological diagnosis with further confirmation of origin by immunostains.
SUMMARY
It is important to correctly identify the background neural stromal fragments as they are an important clue in identification of the lesion. These can be easily missed possibly due to more attention given to the abundant large cells in the foreground. However, FNAC or core biopsy may miss the scant immature neuroblastic component; thereby, a complete resection is recommended due to prognostic and therapeutic implications.
COMPETING INTERESTS STATEMENT BY ALL AUTHORS
The authors declare that they have no competing interests.
AUTHORSHIP STATEMENT BY ALL AUTHORS
Each author has participated sufficiently in the work and take public responsibility for appropriate portions of the content of this article.
All authors read and approved the final manuscript.
Each author acknowledges that this final version was read and approved.
ETHICS STATEMENT BY ALL AUTHORS
As this is case without identifiers, our institution does not require approval from Institutional Review Board (IRB) (or its equivalent).
LIST OF ABBREVIATIONS (In alphabetic order)
FNA - Fine Needle Aspiration,
FNAC - Fine Needle Aspiration Cytology,
GN - Ganglioneuroma.
EDITORIAL/PEER-REVIEW STATEMENT
To ensure the integrity and highest quality of CytoJournal publications, the review process of this manuscript was conducted under a double-blind model (authors are blinded for reviewers and vice versa) through automatic online system.
REFERENCES
- A5-year-old girl with a congenital ganglioneuroma diagnosed by fine needle aspiration biopsy: A case report. Cytojournal. 2008;5:5.
- [Google Scholar]
- An interesting case of differentiated neuroblastoma-ganglioneuroma of the neck in a 5 year old female child. J Evol Med Dent Sci. 2013;2:4298-301.
- [Google Scholar]
- Peripheral neuroblastic tumors: Pathologic classification based on recommendations of international neuroblastoma pathology committee (Modification of shimada classification) Pediatr Dev Pathol. 2000;3:184-99.
- [Google Scholar]
- Cervical ganglioneuroma: Report of a case. Otolaryngol Head Neck Surg. 2001;124:115-6.
- [Google Scholar]
- Orbital ganglioneuroma in a patient with chronic progressive proptosis. Arch Ophthalmol. 2004;122:1712-4.
- [Google Scholar]
- Ganglioneuroma of the internal auditory canal: A case report. Audiol Neurootol. 2007;12:160-4.
- [Google Scholar]
- Primary cutaneous ganglioneuroma: A report of two cases and literature review. Am J Dermatopathol. 2003;25:239-42.
- [Google Scholar]
- Fine needle aspiration cytology of pseudosarcomatous reactive proliferative lesions of soft tissue. Acta Cytol. 2002;46:1049-55.
- [Google Scholar]







