Translate this page into:
Drug eluting beads on cytology smears
-
Received: ,
Accepted: ,
This is an open-access article distributed under the terms of the Creative Commons Attribution-Noncommercial-Share Alike 3.0 Unported, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
To the Editor,
Transarterial chemoembolization (TACE) is the most widely used primary treatment for unresectable hepatocellular carcinoma (HCC). TACE increases the in-situ dwell time and concentration of drug through vascular occlusion by drug-eluting beads (DEB). DEB consist of injectable polymeric microspheres of calibrated size that can be loaded with various antineoplastic solutions.[1]
We describe here the appearance of doxorubicin drug eluding beads on cytology in a 60-year-old African-American male with a past medical history of hepatitis C, hypertension, HCC, hypothyroidism, and arthritis. The patient underwent three TACE procedures within the year for treatment of HCC. Four months after the last chemoembolization, a computed tomography (CT) scan showed a suspicious lesion next to the TACE area. An ultrasound guided fine needle aspiration and core biopsies were done of the suspicious lesion.
The cytology showed moderately cellular smears composed of groups of neoplastic cells with endothelial wrapping consistent with HCC. Intermixed with hepatocytes were circumscribed dense eosinophilic globules consistent with the DEB from chemoembolization [Figures 1–3], done 4 months ago. The core biopsy showed nests of malignant cells with focal pseudoacinar pattern, in background of cirrhosis. On reticulin stain the tumor showed decreased staining with thickened trabeculae confirming the diagnosis of HCC seen on smears. A total of four fine needle passes and two 18 gauge core biopsies were done. The chemoembolization beads were seen only in one air dried smear.
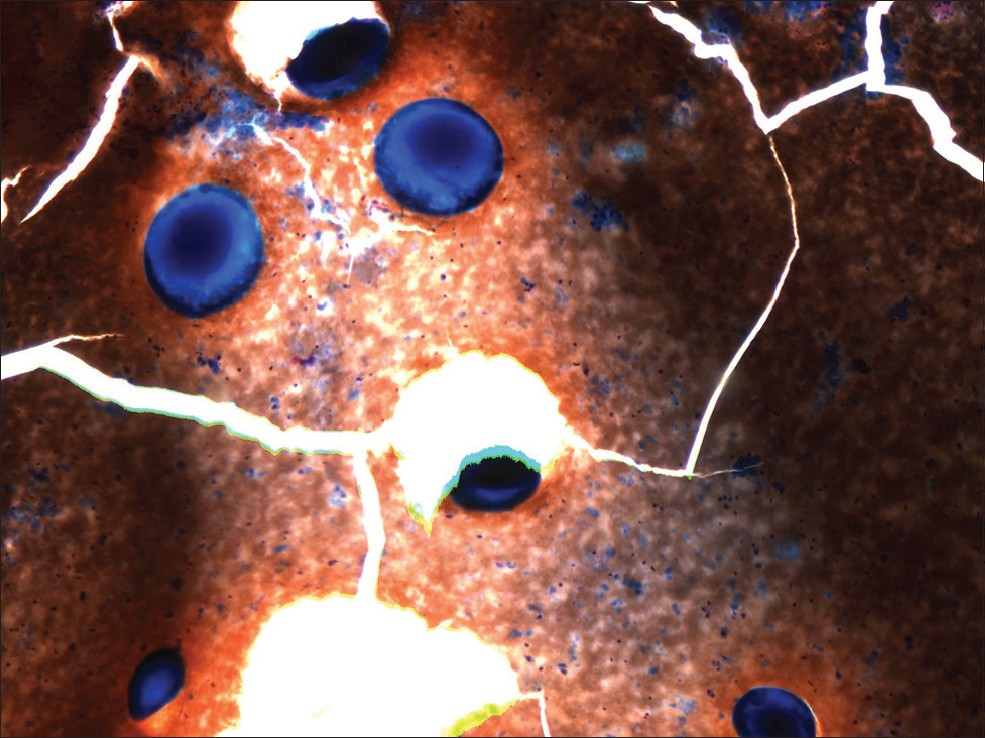
- Drug eluting beads on cytology smear (4× diff quik stain)
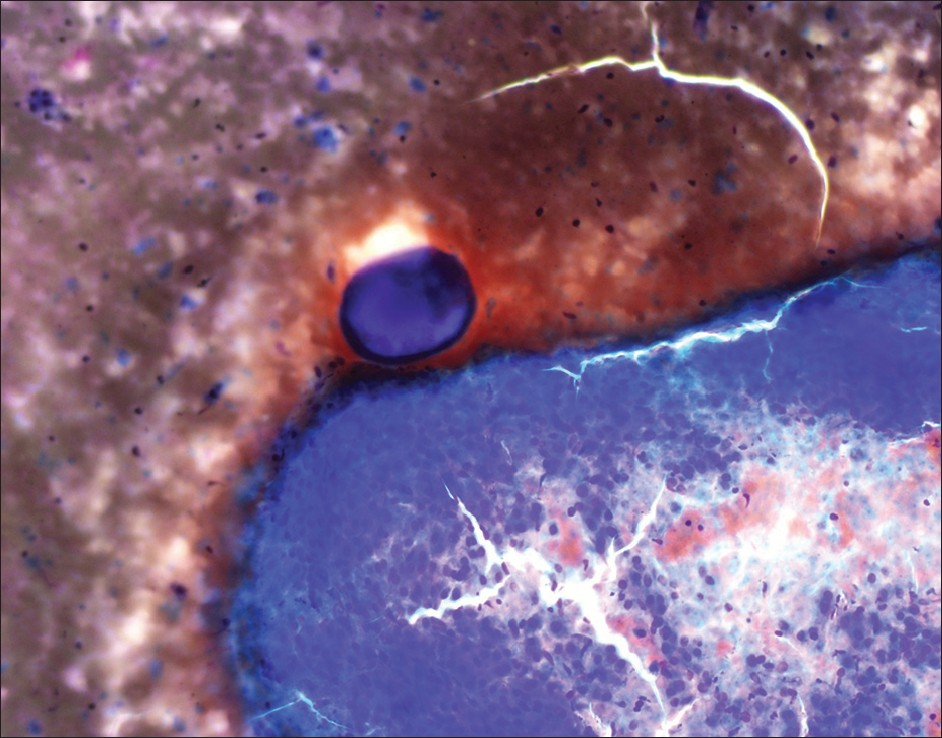
- Drug eluting beads on cytology smear (4× diff quik stain)
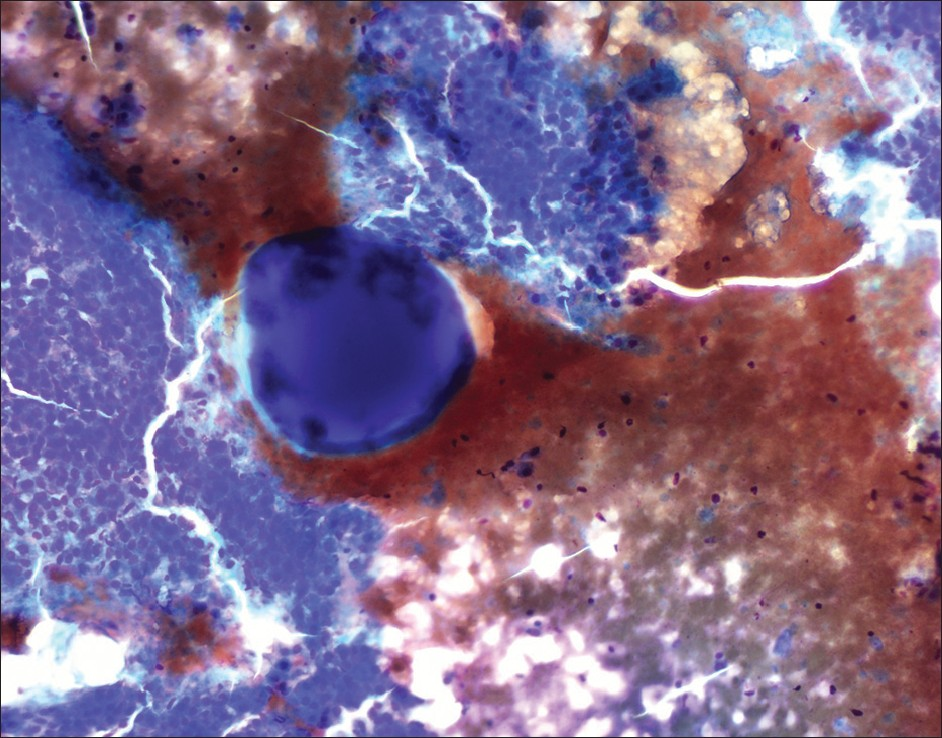
- drug eluting beads on cytology smear (4× diff quik stain)
Developed in mid-2000, DEB can be loaded with cytotoxic drugs for the chemoembolization of hypervascular tumors.[2] These beads slowly release the cytotoxic drug in a controlled fashion into the tumor, inflicting local ischemia while reducing systemic drug concentrations.[2] In our patient the doxorubicin eluting beads were used. These were seen as homogenous, well circumscribed purple, foreign body globules measuring in size from 100–300 μm on air dried cytology smears stained with Romanowsky stain [Figures 1–3]. Previously described microscopic appearance of drug eluting and radioactive beads has been reported in histology tissue sections.[13–5] The rationale of using these DEB is based on the assumption that the vector releases its chemotherapeutic agent, which is able to diffuse locally in the embolized area and causes the necrosis of the target tissue.[1]
The tissue adjacent to beads shows characteristic coagulative necrosis and an inflammatory–fibrotic reaction few weeks after the procedure. The DEB have been demonstrated in the tissue sections from explanted liver, but to our knowledge they have not yet been described in a cytology preparation. In the current case we did see a foreign body type giant cell [Figure 4] but did not see any necrosis or fibro-inflammatory reaction adjacent to the beads.
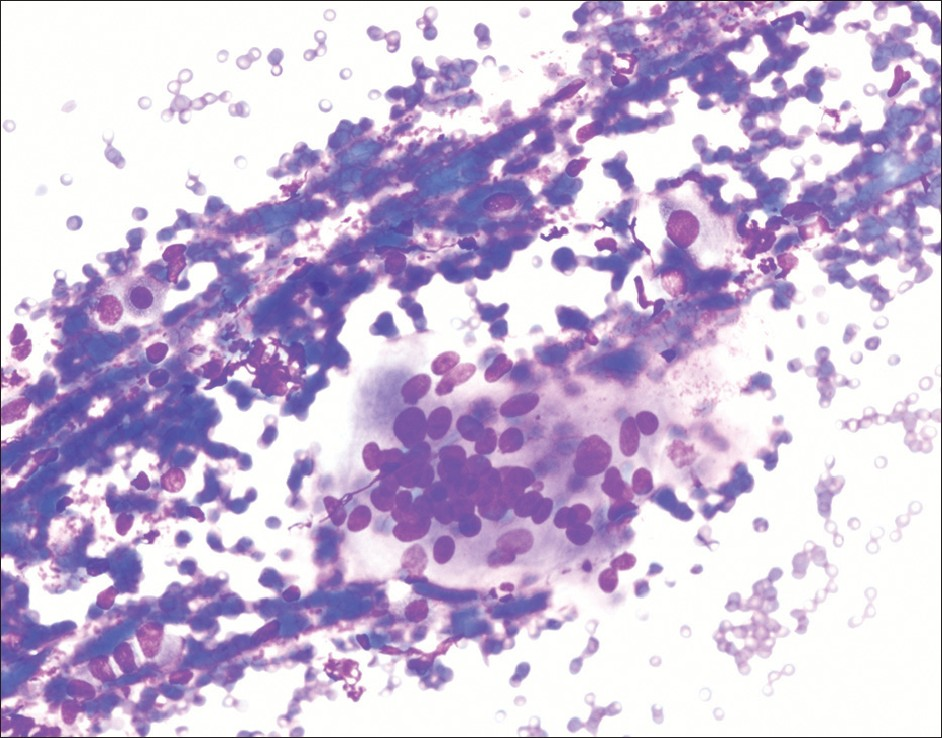
- Foreign body type of giant cell (400× diff quik stain)
COMPETING INTEREST STATEMENT BY ALL AUTHORS
The authors declare that they have no competing interests.
AUTHORSHIP STATEMENT BY ALL AUTHORS
All authors of this article declare that they qualify for authorship as defined by the ICMJE. All authors are responsible for the conception of this study, have participated in its design and coordination, and helped to draft the manuscript. All authors have read and approved the final manuscript.
ETHICS STATEMENT BY ALL AUTHORS
As this is a case report in the form of a letter without patient identifiers, approval from the Institutional Review Board (IRB) is not required.
EDITORIAL / PEER-REVIEW STATEMENT
To ensure the integrity and highest quality of CytoJournal publications, the review process of this manuscript was conducted under a double blind model (authors are blinded for reviewers and vice versa) through automatic online system.
Available FREE in open access from: http://www.cytojournal.com/text.asp?2012/9/1/23/102866
REFERENCES
- Embolization of hepatocellular carcinoma with drug-eluting beads: Doxorubicin tissue concentration and distribution in patient liver explants. J Hepatol. 2011;55:1332-8.
- [Google Scholar]
- DC bead: In vitro characterization of a drug-delivery device for transarterial chemoembolization. J Vasc Interv Radiol. 2006;17:335-42.
- [Google Scholar]
- Transarterial chemoembolization with epirubicin-eluting beads versus transarterial embolization before liver transplantation for hepatocellular carcinoma. J Vasc Interv Radiol. 2010;21:327-32.
- [Google Scholar]
- Pathologic evaluation of a spherical polyvinyl alcohol embolic agent in a porcine renal model. J Vasc Interv Radiol. 2003;14:89-98.
- [Google Scholar]
- Gastroduodenitis associated with yttrium 90-microsphere selective internal radiation: An iatrogenic complication in need of recognition. Arch Pathol Lab Med. 2008;132:1734-8.
- [Google Scholar]







